Everything you need to know about stem cells
What are stem cells, and what makes them so unique? What are the different types of stem cells, and how have they impacted modern medical science? Here is us answering all your questions about stem cells.

The vaccine technology has been a fast evolving field of science. Since the invention of the first vaccine by Edward Jenner against cowpox over 300 years ago, we have indeed come a long way with there being a vaccine against several commonly occurring infections.
Interestingly, when we hear vaccine, we think infection. However, what if we could be vaccinated for other diseases, like say cancer?
As improbable as this sounds, the research community is slowly inching forward to make this a reality, with a few approved cancer vaccines already in the market. Let us take a closer look at these vaccines, along with a specific vaccine candidate that may hold special potential in the future of cancer vaccines.
A vaccine is a combination of biological and chemical material that is used to provide immunity against infections. It works by introducing dead, weakened, or bits and pieces of the pathogen into the body, thereby training the immune system to recognise and eliminate the pathogen before the real, deadly version pays a visit!
It is easy to imagine creating a vaccine against something that is coming from the outside, like viruses or bacteria. But how do we create a vaccine for something like cancer, which grows within our own body and is made up of the very same cells as the rest of the body?
The answer lies in the uniqueness of cancer cells. Although cancer cells are born out of the normal, healthy cells in our body, they usually make less of, or more of, or modified versions of specific proteins when compared to the healthy cells. This is what causes them to lose control and divide uncontrollably in the first place. Cancer vaccines hack this difference - the Achilles’ heel of the cancer cell, and help train one’s own immune system in eliminating their cancerous cells.
Cancer vaccines can be preventative or therapeutic (Grimmett et al., 2022).
Preventative cancer vaccines, as the name suggests, are used to prevent cancers of certain type. As of now, preventative vaccines have only been created for cancers caused by viruses - Ex: Hepatocellular cancer and cervical cancer. These vaccines work in the same way as regular vaccines.
Therapeutic cancer vaccines are given after cancer has already been diagnosed. However, it helps prevent further progression of the disease. An example for this is Sipuleucel-T which is used for prostate cancer. The vaccine targets a specific enzyme called PAP (Prostate acid phosphatase) which is made in increased amounts by prostate cancer cells.
With the initial success of these vaccines, several vaccine candidates for cancers such as pancreatic and prostate cancer, brain tumour and breast cancer are now being tested in clinical trials.
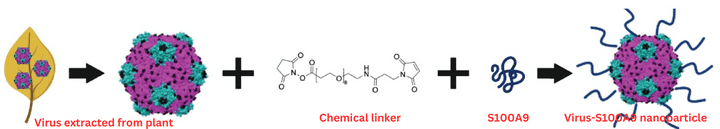
The cowpea mosaic virus (CPMV) is extracted from plants and chemically linked to the S100A9 protein to create the virus nanoparticle. Credit: Young Hun Chung et al., 2023 CC BY-NC-ND.
An interesting example of therapeutic cancer vaccine is seen in a recent research work published in the journal Proceedings of the National Academy of Sciences (PNAS) (Chung et al., 2023). The team focused on targeting a specific protein called S100A9 which is found in large quantities in the tissue spaces surrounding tumours (called tumour microenvironment). Increased amount of this protein has been found in many cancers including gastric, breast and pancreatic cancer. More interestingly, this protein has also been found in locations far off from the actual tumour, such as the lungs. However, the protein doesn’t sit there quietly. As a matter of fact, these proteins invite the tumour cells growing in far off locations to come and settle with them in the lungs.
In more scientific terms, S100A9 acts as a chemoattractant, helping cancer metastasise to the lungs.
The group hence decided to target this protein. In order to do so, they used viruses that infect plants (and hence cannot infect humans). They used the cowpea mosaic virus (CPMV) and other virus like particles as nanoparticles, and conjugated or attached the S100A9 protein to the virus nanoparticle. The idea was that when these S100A9 carrying viruses were introduced into the body, it would trigger the production of antibodies against S100A9. This would reduce S100A9 in the lungs, thereby leading to lesser lung metastasis.
To test this idea, the group injected the viruses into mice that were modelled to study skin cancer metastasis. Interestingly, the mice showed up to 10-fold reduction in lung metastasis. The group obtained similar results when they tested breast cancer metastasis to the lungs.
The team therefore concluded that the vaccine was triggering an immune response against S100A9, which in turn was leading to reduced metastasis to the lungs in skin and breast cancer.
Cancers are really hard to treat, mostly because one individual’s cancer type can be very different from another individual’s type. Therefore, personalised medicine that can specifically target an individual’s unique cancer type is perhaps the future of cancer treatment. Therefore, studies like this hold immense potential in the future of cancer treatment, as it taps into the potential of one’s own immune system in killing their cancer cells.