Everything you need to know about stem cells
What are stem cells, and what makes them so unique? What are the different types of stem cells, and how have they impacted modern medical science? Here is us answering all your questions about stem cells.
Pain is an interesting phenomenon involving quick coordination between many parts of our body. When we encounter a harmful stimulus, for example, let’s say we accidentally touch a hot pan, our brain, in a fraction of a second, recognises that something is wrong and responds by producing a sharp unpleasant sensation of pain. This is our brain’s way of telling us - ‘Hey! Keep your hands away from that object.’ This helps us be more careful around hot pans in the future. Pain, as odd as it sounds, for the vast majority, is good for us. It is protective in nature.
However, in some cases, pain can take a life of its own and can turn chronic. Chronic pain is defined as the pain that lasts for more than 3 months, beyond the regular recovery period. Such kind of pain takes a detour from the regular pain pathway and can be triggered even without any kind of painful stimulus. It, therefore, is no more protective and can be considered a disease in its own right.
Chronic pain is a global medical health problem, affecting over 100 million adults in the United States alone. Besides the obvious suffering, chronic pain can reduce productivity and also bring with it heavy medical costs. A therapy, called the Scrambler Therapy, that has gained traction in the past few years may harbour new hope for many patients with chronic pain (Smith et al., 2023).
Pain, as we all know it, is the distressing sensation, most often caused due to some kind of tissue damage. Its main purpose is to caution our body to take action and prevent any further damage.
But how exactly do we feel this pain? Let’s once again consider the example we saw previously. When we touch something hot, it immediately activates specific nerve endings present under our skin called nociceptors. These activated nociceptors carry this ‘hot’ information in the form of electrochemical signals to the spinal cord. From the spinal cord, the signals are sent to different parts of the brain. It is the activation of the brain that produces the deep, miserable sensation of pain. This type of pain lasts for a short duration of time and resolves once the damage is resolved and is called acute pain.
On the other hand, certain conditions, like injury and inflammation, may lead to a deviation from this normal pain pathway. This results in a different kind of pain, called chronic pain, that persists beyond recovery.
Chronic pain is the kind of pain that lasts for more than 3–6 months. In these cases, nerve cells have been shown to become hyper-excited and trigger pain signals even in the absence of painful stimuli. Certain types of injuries, chemotherapy, specific viral infections and conditions like multiple sclerosis and cancer can cause chronic pain.
Unfortunately, many of the pain relief medicines are not always effective against chronic pain, leading to a lifelong struggle for several patients (Yam et al., 2018).
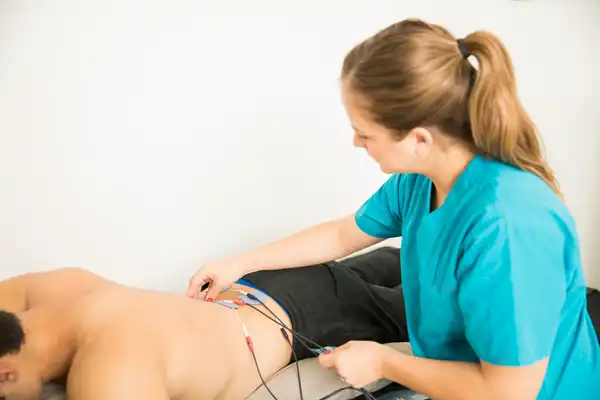
. Scrambler Therapy involves placing electrodes around the area of pain. Credit: [Freepik](https://www.freepik.com/free-photo/electro-stimulation-physical-therapy-young-woman_1318981.htm).](/static/2ee869a7bb422ac40a488a2ef5616183/80e3c/scrambler_therapy.jpg)
Scrambler Therapy involves placing electrodes around the area of pain. Credit: Freepik.
Scrambler Therapy, developed by a pain physician named Giuseppe Marineo, uses electrical stimulation to treat chronic pain. The treatment protocol involves first identifying the region of pain. Electrodes are then placed on the normal/non-painful tissue surrounding the painful region. This region is then subjected to mild electrical stimulation for 30–45 minutes. This results in the stimulation of the nerve endings in the non-painful region. It is proposed that this causes the pain information conducted by the painful tissue to be replaced by the non-pain signals produced by the electrical device.
Patients report a soothing sensation after each session and with subsequent sessions, usually given for a period of 2 weeks, patients experience long-lasting pain relief. The treatment tends to confuse or rather retrain the brain to no longer perceive the region to be painful. If the pain reappears, patients can be given booster sessions (Majithia et al., 2016).
With the first clinical trial conducted by Giuseppe Marineo on terminally ill cancer patients in 2003, studies have now extended to treat chemotherapy induced pain, chronic lower back pain and post surgical pain, to name a few. Some reviews of these trials show that approximately 80-90% of patients benefit from the therapy (Smith et al., 2023).
Although further clinical trials are required to fully confirm the effectiveness of this therapy, several pain-struck patients now have a new ray of hope to hold on to (Marineo, 2019).